Positron Emission Tomography (PET) combined with Computed Tomography (CT) provides a unique, non-invasive, and highly accurate imaging technique that allows clinicians to observe functional changes in the body. This advanced imaging method offers both detailed anatomical and metabolic information, giving a comprehensive picture of a patient's health.
PET works by using a small amount of radioactive material to track metabolic activity within the body. The most commonly used radioactive tracer worldwide is 18F-FDG, a glucose analog. This substance is preferentially absorbed by cells with higher metabolic activity, such as cancer cells. Therefore, areas with abnormal or increased metabolic activity, such as tumors, will appear "hotter" (highlighted) in the scan.
The procedure itself is safe, with relatively low radiation exposure, and can provide invaluable information for diagnosing and monitoring various conditions.
Oncological Indications:
Cancer Management: PET/CT scans are beneficial in the staging of cancer, assessing the extent of the disease, and evaluating how well a tumor is responding to treatment. It is also crucial for restaging and surveillance to monitor for potential recurrence.
Non-Oncological Indications:
Dementia: PET/CT can help assess brain function, aiding in the diagnosis of conditions like Alzheimer’s disease and other forms of dementia.
Epilepsy: For patients with epilepsy, PET/CT can help pinpoint the origin of seizures and guide appropriate treatment options.
Fever of Unknown Origin: In cases where the cause of fever cannot be determined, PET/CT imaging can help identify underlying infections or inflammatory diseases.
Cardiac Viability: PET/CT scans are used in cardiology to evaluate heart function, particularly in assessing areas of the heart that may still be viable after a heart attack.
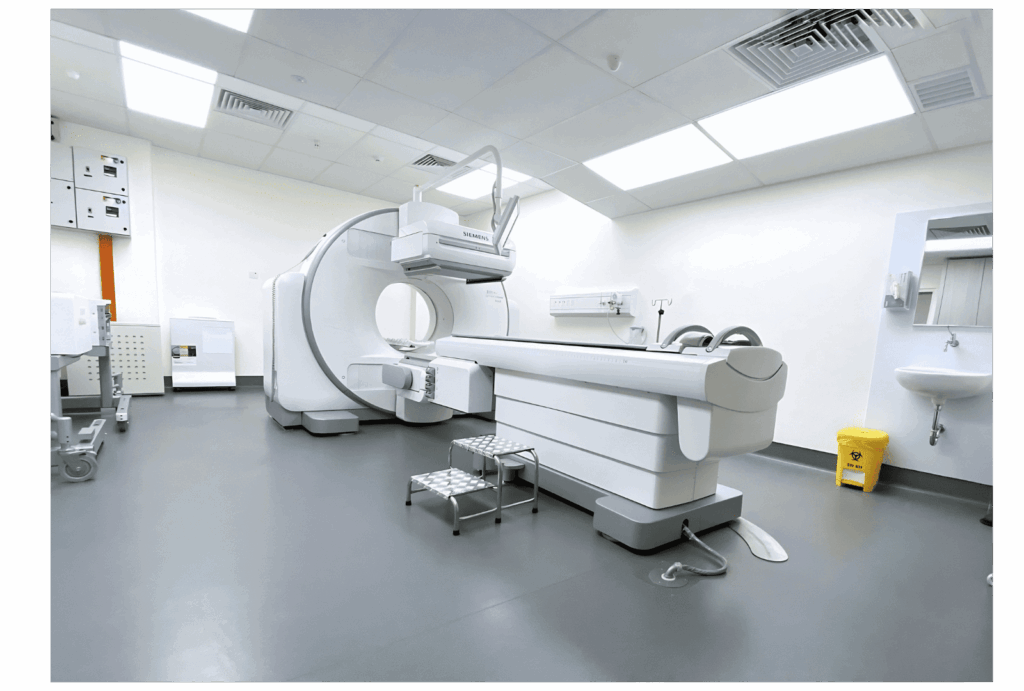
Single Photon Emission Computed Tomography (SPECT-CT) is a hybrid imaging technique that combines the functional imaging capabilities of SPECT with the detailed anatomical information from CT. This advanced imaging modality provides sensitive, precise, and targeted insights into how different parts of the body are functioning.
While similar to PET-CT, SPECT-CT has the advantage of being able to perform a broader range of imaging studies, using different types of radioactive tracers to assess various physiological processes. Like PET-CT, the procedure is very safe, and the radiation exposure from the scan is relatively low.
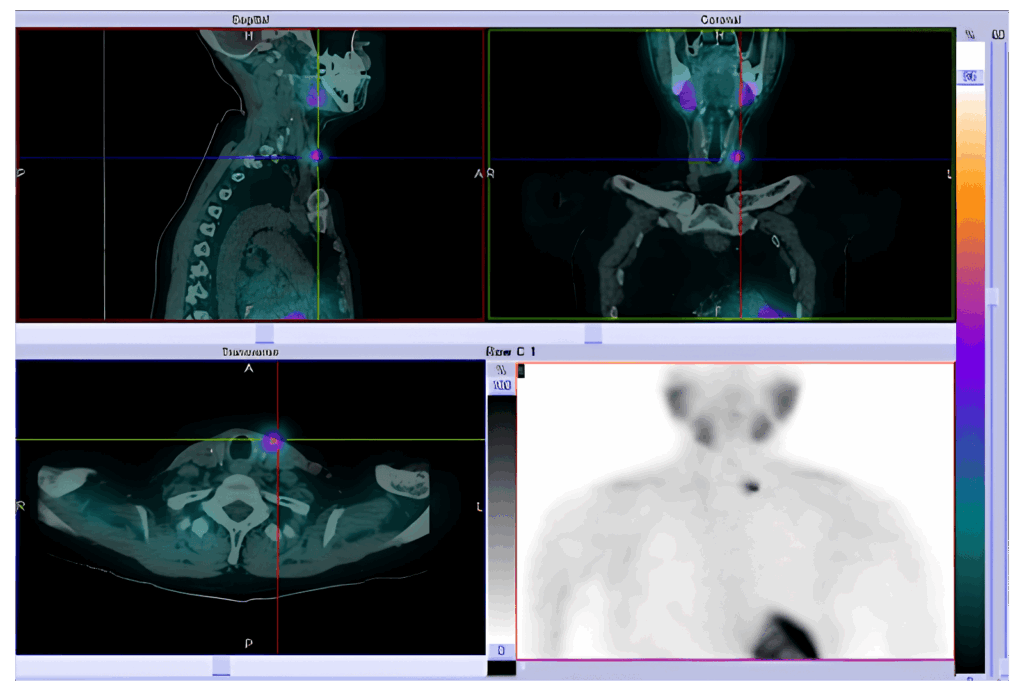
Heart Imaging:
Bone Imaging: Identifies areas of bone inflammation, infection, or abnormalities, such as in cases of fractures, infections, or bone cancer.
Renal Imaging:
Lung Perfusion Imaging: Evaluates blood flow in the lungs, helping detect conditions like pulmonary embolism or other pulmonary disorders.
Gastrointestinal-Related Imaging:
Endocrine Imaging:
Whole Body I-131 Post-Therapy Imaging: Used for post-therapy monitoring of thyroid cancer, assessing the spread of cancer cells or the effectiveness of treatment.
A type of nuclear medicine treatment that uses radioactive iodine to target and destroy thyroid cells. This therapy is primarily used to treat hyperthyroidism and thyroid cancer.
Hyperthyroidism occurs when the thyroid gland produces an excess of hormones, either due to hyperfunctioning nodules or overactive thyroid tissue. Radioiodine-131 is uniquely effective because it targets and destroys these hyperfunctioning thyroid cells while sparing the healthy thyroid tissue. As a result, this therapy helps restore normal thyroid function by reducing hormone production to appropriate levels.
In the case of thyroid cancer, Radioiodine-131 therapy is commonly used after the surgical removal of the thyroid gland. The therapy works by targeting and eliminating any remaining thyroid cells or metastatic thyroid tissue that might have spread to other parts of the body. This minimizes the risk of cancer recurrence and helps ensure that any residual cancerous cells are destroyed.
The radioactive iodine is typically administered orally in the form of a capsule or liquid. It is absorbed by the body and specifically targeted to the thyroid tissue. Once the iodine reaches the thyroid, it emits radiation that destroys the targeted thyroid cells. Since it is a targeted therapy, only the thyroid tissue is affected, and surrounding healthy tissues are spared.




Lutetium-177 PSMA (Prostate-Specific Membrane Antigen) Therapy is an advanced form of nuclear medicine therapy designed to target and treat metastatic prostate cancer. This therapy uses Lutetium-177, a radioactive isotope, to specifically target prostate cancer cells that have spread to other areas of the body, such as lymph nodes and bones.
The treatment works by attaching the radioactive Lutetium-177 to a molecule that binds to PSMA, a protein found in high amounts on the surface of prostate cancer cells. Once the Lutetium-177 is delivered to the cancer cells, it emits radiation that destroys these cancerous cells while minimizing damage to surrounding healthy tissues.
Lutetium-177 PSMA therapy is targeted and precision-based, meaning that it focuses specifically on the metastatic prostate cancer cells, making it an effective treatment for patients with advanced prostate cancer. It is especially useful for cases where cancer has spread to other parts of the body, such as the bones or lymph nodes.
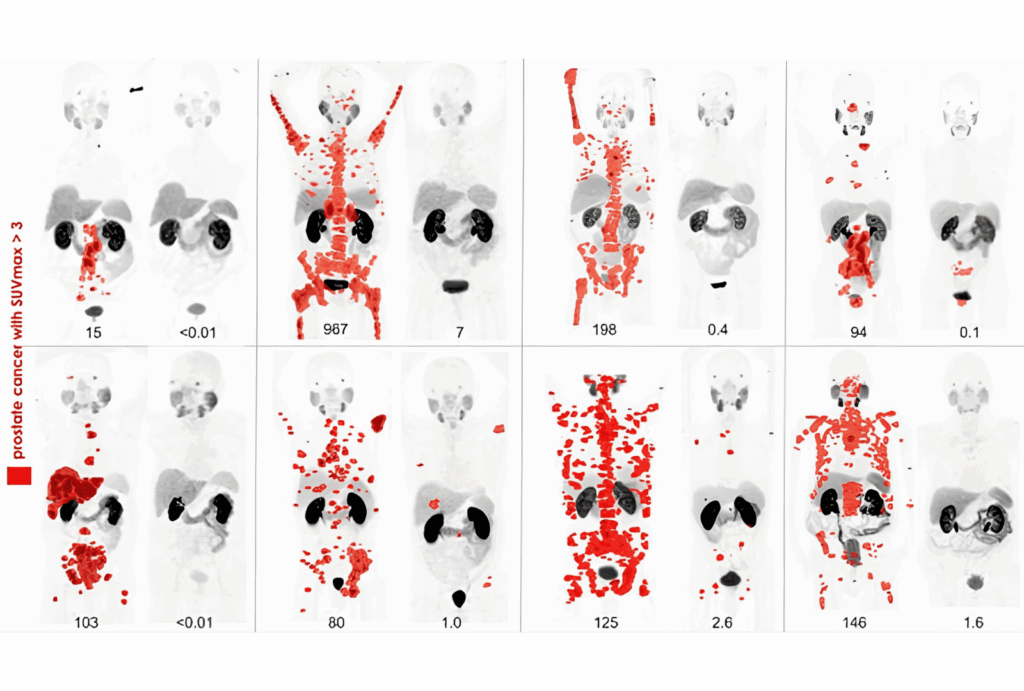
2018 Annual Meeting of the Society of Nuclear Medicine and Molecular Imaging (SNMMI) Image of the Year Award,
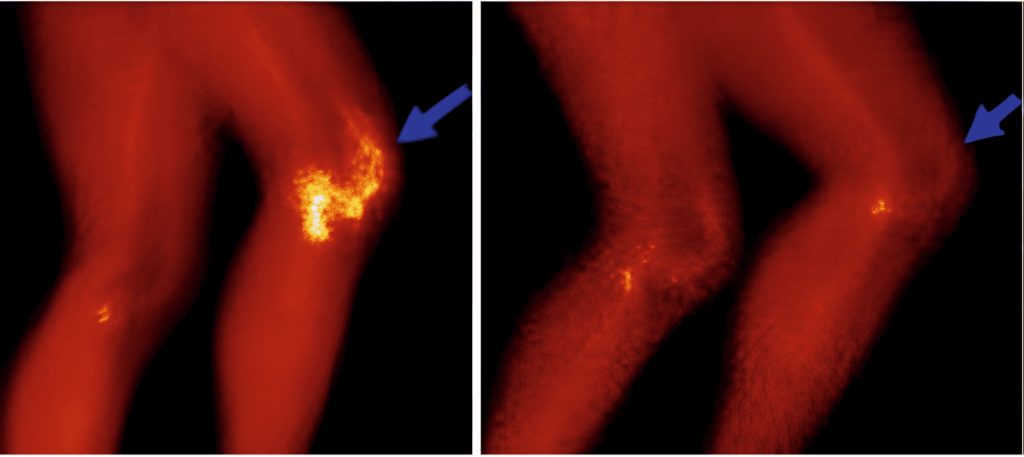
Radiosynovectomy is a targeted nuclear medicine treatment used to treat painful joints caused by synovitis—inflammation of the synovial membrane, which lines the joints. This therapy involves the injection of a radioactive substance directly into the affected joint. The radioactive material is carefully selected to ensure it only travels a very short distance which means it can effectively destroy the inflamed synovial tissue without causing damage to surrounding healthy tissues.
The treatment works by targeting the abnormal synovial cells, destroying the inflamed tissue, and thus reducing joint inflammation, pain, and deformity. Radiosynovectomy can significantly improve mobility and quality of life for patients suffering from chronic joint pain caused by diseases like rheumatoid arthritis or other forms of inflammatory arthritis.
Bone Palliation Radionuclide Therapy is used to treat bone metastases—a common complication of cancers such as prostate cancer, breast cancer, and other solid tumors. Bone metastasis can be particularly painful, affecting the bones and causing significant discomfort for patients. When metastasis is widespread, treatment options are focused on relieving pain and improving quality of life.
In cases of extensive bone metastases, radiopharmaceuticals such as strontium-89, radium-223, and samarium-153 are used for targeted therapy. These radioactive substances are selectively absorbed by bone tissue, where they emit radiation that targets and destroys the cancerous cells, helping to alleviate bone pain associated with metastasis. This form of therapy is effective in reducing symptoms, improving mobility, and enhancing overall quality of life for patients.
Both Radiosynovectomy and Bone Palliation Radionuclide Therapy are safe, non-invasive treatments administered under the supervision of a Nuclear Medicine Physician. These therapies are designed to improve the quality of life for patients, providing targeted relief with minimal risks and side effect
Monday - Thursday: 8:30am - 5:00pm
Friday: 8:30am - 4:30pm
Saturday & Sunday: Closed
Malaysia Website Design, Lightflex.